

This excerpt taken from Dr. Campbell’s The Future of Nutrition (2020) explains why breadth of effect is critical when assessing health and nutrition protocols, and explores how the current reductionist medical paradigm ignores this criterion. To learn more about The Future of Nutrition, read our dedicated webpage. To learn more about reductionism and its alternative, wholism, read our webpage on Whole.
By embracing the vast interconnection of research topics, wholism does not exclusively seek clear-cut, black-and-white answers. Rather, wholism encourages the humble acceptance of our own continually evolving ignorance—the idea that each new research finding contributes to a greater understanding of the world (or sheds light on previous misunderstanding) and how we might more effectively thrive within it. Wholism strives toward a more complete understanding of the vast integrative systems that characterize our bodies, our environments, our societies, and the like, but highlights that we can only ever strive, and never reach a hard-and-fast final answer. In this striving, wholism does not compromise our standards of evidence. If anything, it demands an even higher standard of evidence than the current one. It does not reject evidence, but demands that we consider the whole body of evidence. It encourages us to use a wide array of study types, and to understand the appropriateness of certain types of studies for certain subjects and the inappropriateness of other study types for other subjects. It encourages us to interpret this wide array of study types not only as isolated and distinct events but also as parts of a larger whole.
Wholism does not reject Hill’s useful criteria for the evaluation of epidemiological evidence. On the contrary, it celebrates and bolsters them by adding a new, tenth criterion: breadth.
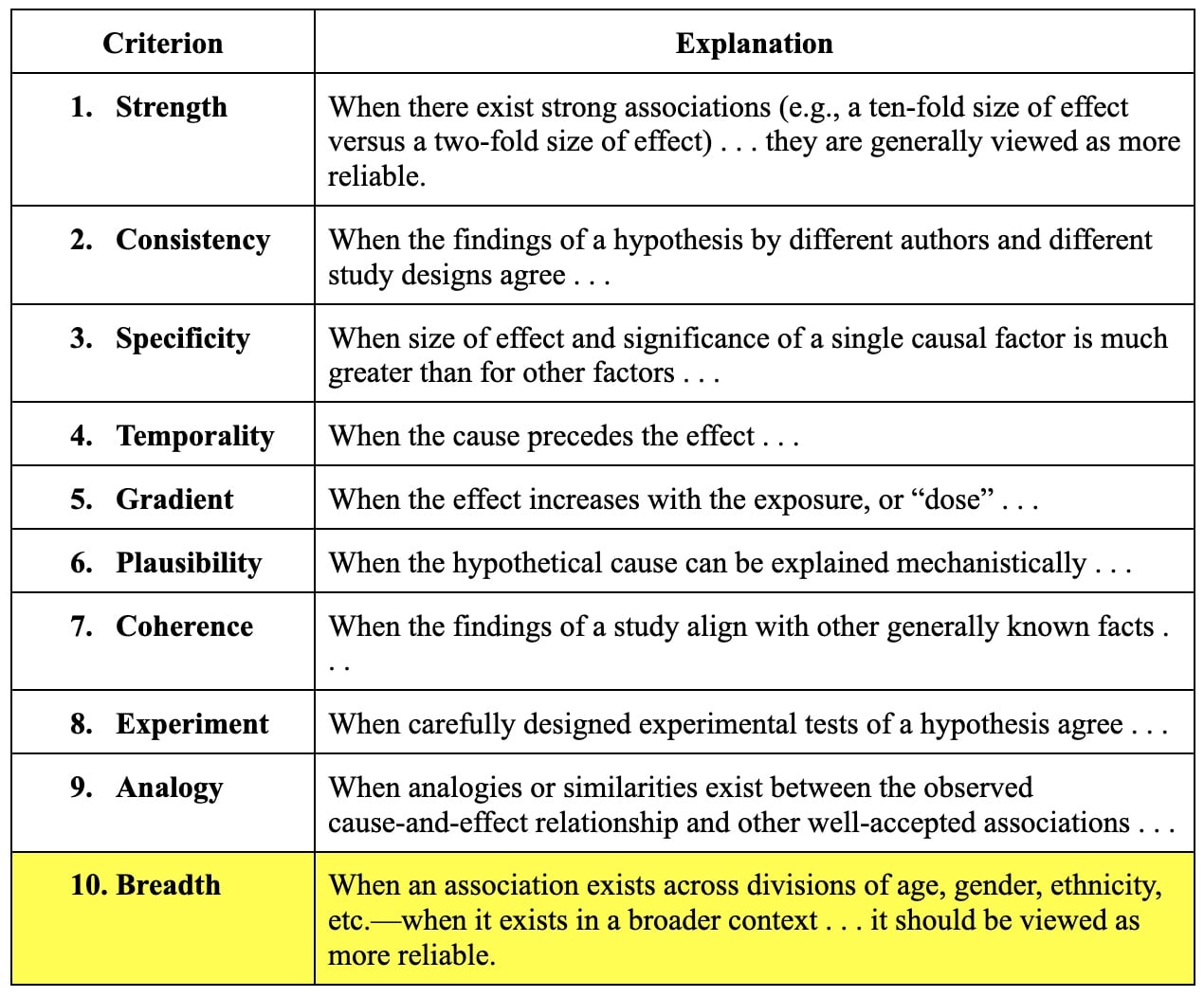
Breadth of effect is especially important in the case of nutritional effects, which I will discuss in greater depth in chapter eight. Breadth asks whether an intervention might be used to treat a fuller range of illness and disease; it asks whether recommendations might apply, at least in part, for everyone, regardless of age, ethnicity, and sex; and crucially, it asks whether an intervention may be capable of both treating and preventing disease. In short, this single addition makes a huge difference. Emphasizing breadth of effect results in a profound departure from current pharmacologic treatment protocols, which almost exclusively target the alleviation of individual symptoms on an illness-by-illness basis, and even on a treatment-by-treatment basis within a single illness!
Again, this should not be taken as a repudiation of the original nine criteria. No doubt, Hill’s original criteria are very useful. But they also conform to a reductionist model of disease causation. By adding breadth—that is, by refocusing our attention on the whole—we correct this issue. Whereas a reductionist assessment of evidence can be misleading and even potentially dangerous, breadth is far more discerning. For example, there may be very compelling evidence indicating a certain diet’s ability to promote weight loss, and that evidence could very well satisfy most of the nine old criteria. But what if that diet also had adverse effects on other measures of health? What if it also promoted loss of strength or loss of balance among older adults? What if it only resulted in weight loss for young women, and did not have a similarly beneficial effect for older men? Obviously, we would prefer a diet whose positive effects worked across the board, so why would we not consider the evidence for an intervention in an across-the-board way, too?
The point I’m circling again and again is that good evidence should satisfy the principles of both reductionism and wholism. Though there’s an obvious value in knowing how certain mechanisms work and how certain interventions influence those mechanisms, this knowledge must also be meaningful within a broader context. If a piece of “good” evidence cannot help to clarify the true nature of the whole, then it doesn’t matter how well it delineates a specific mechanism. If we are committed to truly useful science, then we must keep our eyes on the prize—the whole prize—and not let ourselves slip into a self-congratulatory cycle of highly specialized quests for trivia that the public can neither understand nor use.
Or, to put it more mildly, we need balance.
The Future of Nutrition: An Insider’s Look at the Science, Why We Keep Getting It Wrong, and How to Start Getting It Right
In The Future of Nutrition, T. Colin Campbell cuts through the noise with an in-depth analysis of our historical relationship to the food we eat, the source of our present information overload, and what our current path means for the future—both for individual health and society as a whole. The Future of Nutrition offers a fascinating deep-dive behind the curtain of the field of nutrition—with implications both for our health and for the practice of science itself.
Copyright 2024 Center for Nutrition Studies. All rights reserved.